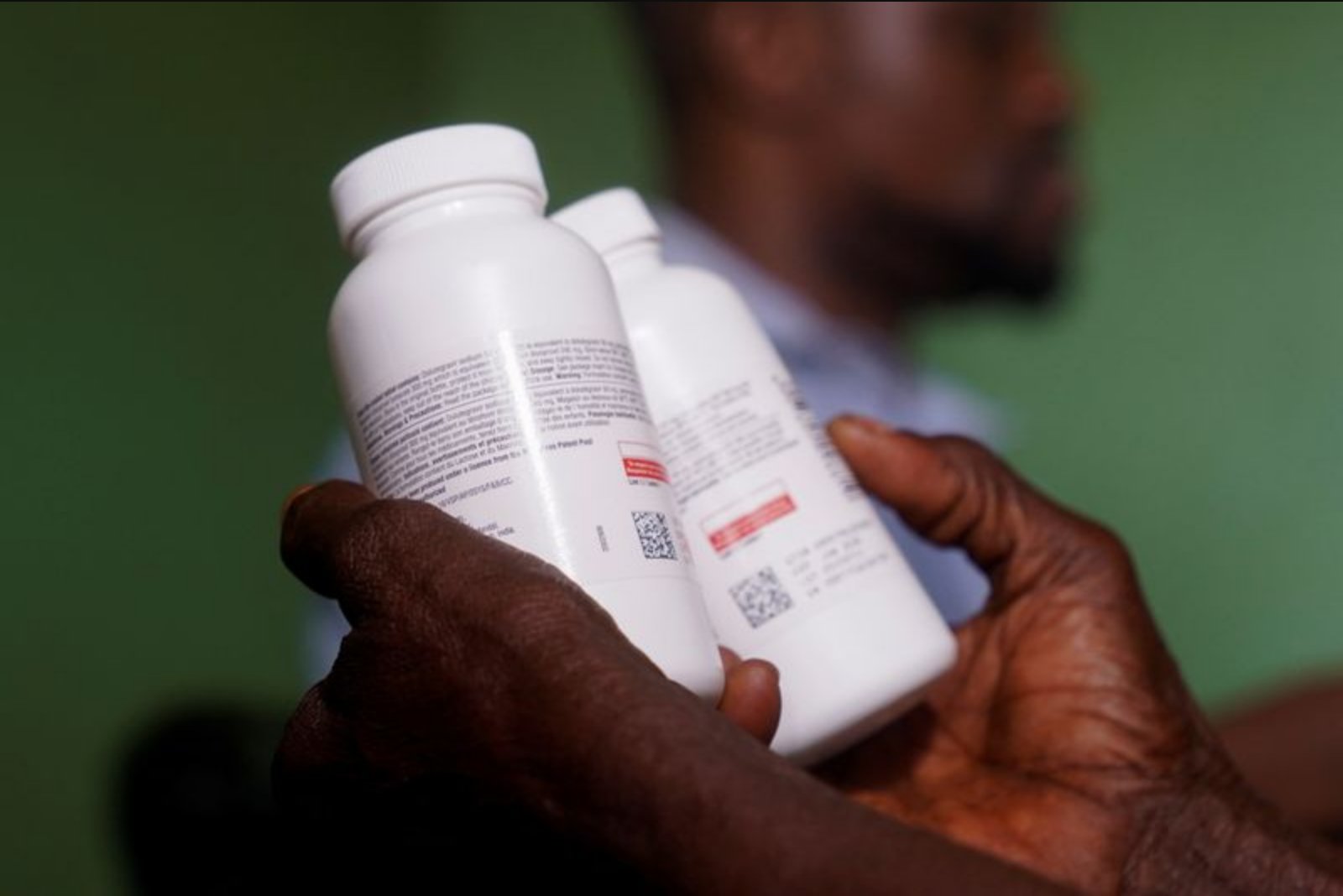
For months after a sudden reduction in foreign assistance, volunteers in Nigeria’s Benue State walked village paths to find and reconnect people living with HIV to life-saving medication.
Josephine Angev, 40, was among those who knocked on doors and made repeated visits to patients whose supply of antiretroviral drugs had run out. She said many people did not appreciate how quickly stopping treatment could endanger their health. "They don’t understand the implications," she said.
When antiretroviral treatment is interrupted, the medication’s suppression of the virus can lapse and the virus can rebound. That puts individuals at risk of HIV-related illnesses within months and increases the chance of onward transmission.
Angev recounted helping a 65-year-old woman who had stopped taking medication after her supplies were exhausted and then became ill. After repeated interventions by Angev, the woman resumed treatment and is now doing well.
How the disruption unfolded
The disruption followed a 90-day pause on foreign aid announced by U.S. President Donald Trump on January 20 last year. The United States historically financed around 90% of Nigeria’s HIV treatment costs and supported health workers delivering services. In the months that followed, patients and aid groups reported dramatic changes in how antiretroviral drugs were dispensed.
Major clinics that had previously provided six-month supplies reduced those dispensations to one- or two-week quantities. In the state capital Makurdi, all 10 treatment centers closed for a month. The World Health Organization warned that medication could run out.
Within six weeks of the initial aid suspension, Nigeria announced a $200 million health funding package that included support for HIV treatment. In February 2025 the U.S. government issued a waiver for "life-saving" aid, including antiretrovirals. Still, volunteers were essential in bridging the gaps while services were disrupted and clinics began to reopen with new funding.
Volunteer response and outcomes
Volunteers tied to the Afrocab community support network, a non-profit operating across the continent, formed a small army of community outreach workers. Dinah Adaga, who coordinates volunteers in Benue State, said the teams used phone calls where possible but resorted to home visits when phone contact failed. "If we couldn’t reach someone by phone, we went to their house - we traced the address and knocked on their door," she said.
Between June and December 2025, volunteers in Benue said they brought more than 1,000 people back into care, including 95 children under five. The volunteers estimate that figure represents everyone who had stopped treatment in February and March.
Their work extended beyond reconnecting patients to medication. Volunteers countered misinformation that had circulated in some communities about prayer 'cures' and other misleading claims. They also encouraged pregnant women to return to antenatal care to protect their infants from HIV transmission.
Krittayawan Boonto, UNAIDS country director in Nigeria, said the absence of reports of deaths linked to lack of antiretrovirals was "for us, a good sign."
Scale and national figures
Nigeria is home to roughly two million people living with HIV, one of the largest national burdens worldwide. Afrocab estimates that Benue, a state of about 4.25 million people, has just over 200,000 individuals on treatment.
Following the aid freeze, a UNAIDS tracker initially suggested that 200,000 fewer Nigerians were receiving treatment. However, by the end of 2025 data showed 1.7 million people on treatment, a slight increase from 2024’s 1.6 million. A U.S. State Department spokesperson said the number of those receiving drugs was "very similar" at the end of 2025 compared with 2024, adding that "The narrative suggesting widespread HIV treatment loss... is inaccurate, misleading and irresponsible." Nigeria’s government did not respond to requests for comment.
Prevention and testing suffered
Despite gains in restoring treatment, prevention services and testing were hit harder and for longer. Bright Oniovokukor, a coordinator with the Civil Society for HIV/AIDS in Nigeria, said the number of people accessing prophylactic drugs to prevent HIV infection fell sharply - from 43,000 in November 2024 to below 6,000 in April 2025. He also reported that condom distribution fell by 55%.
Health officials warned that gaps in prevention could lead to more new infections. Dr Oluwafunke Odunlade, head of the HIV unit at WHO Nigeria, noted that testing was also disrupted, with early figures indicating more than a million fewer people tested for HIV in 2025 compared with 2024. That shortfall in testing means cases may have been missed.
Longer-term funding and program shifts
By December, the United States and Nigeria signed a health agreement covering 2026-2030 that commits the U.S. to contribute $2.1 billion and Nigeria $3 billion. The deal prioritises the HIV response and aims to expand treatment programmes, with Nigeria assuming full funding responsibility over the next five years.
The U.S. has said it will fund only workers "formally recognised within government structures," and the agreement places "a strong emphasis on Christian faith-based healthcare providers," reflecting a policy focus the U.S. says is intended to support Nigeria’s Christian population, which has faced threats from Islamist violence.
Local resolve
Back in Benue, volunteers like Angev plan to continue their outreach work. "It can be exhausting, but we do it so lives that might have been lost are instead restored. And when you see them living better lives and truly changed, that’s when you feel happy," she said.
The experience in Benue underlines how community-level action, coupled with emergency national and international funding, helped avert the worst-case outcomes when large-scale aid flows were interrupted. At the same time, the pause exposed vulnerabilities in prevention, testing and supply chains that public health authorities and funders say will need sustained attention as Nigeria transitions to greater domestic financing for HIV services.